| Risk Factor | What Happens | Potential Outcome |
|---|---|---|
| External Heat (Pads, Saunas) | Accelerates drug release from patch | Rapid systemic absorption |
| High Fever (40°C / 104°F) | Increases serum levels by ~33% | Increased opioid toxicity |
| Strenuous Exercise | Boosts local blood flow to skin | Unexpectedly high drug levels |
How Fentanyl Patches Actually Work
To understand why heat is so dangerous, you first have to understand the delivery system. Fentanyl is a potent synthetic opioid used primarily for chronic pain management in patients who already have a tolerance to opioids. Unlike a pill that you swallow, a transdermal patch-such as the brand Duragesic-creates a "depot" of the drug in the upper layers of your skin.
Once applied, the drug slowly diffuses through the skin and into the capillaries. It doesn't hit its peak concentration (Cmax) immediately; it usually takes between 24 to 72 hours to reach a steady state. The goal is a slow, controlled release that lasts for 72 hours. However, this process relies heavily on skin permeability and local blood flow. When the skin gets hot, the "gate" opens wider, and the drug rushes in.
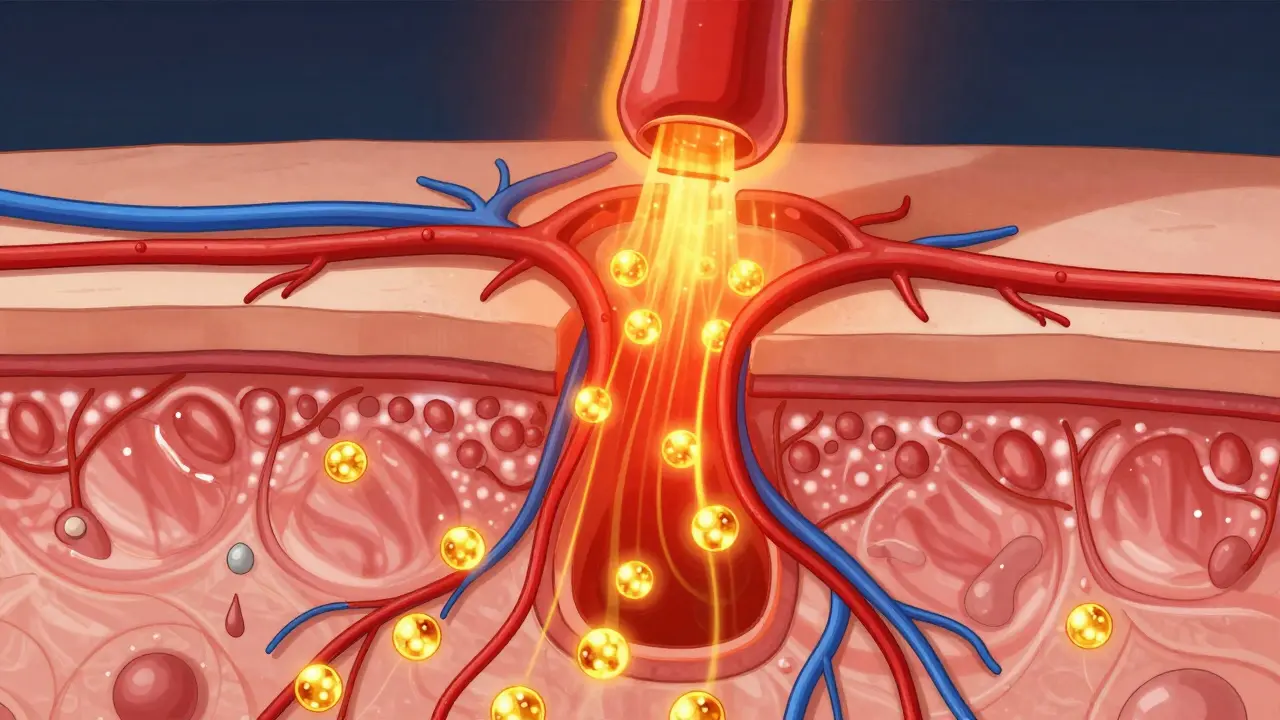
The Science of Heat-Induced Absorption
Heat changes the physics of your skin. When you apply heat, your blood vessels dilate-a process called vasodilation-and local microcirculation increases. Essentially, more blood is flowing under the patch, which means more fentanyl is swept away into your general circulation at a much faster rate.
The numbers are startling. Research has shown that using a controlled heating device to raise skin temperature to about 41°C (105.8°F) for just four hours can increase maximum serum concentrations nearly three-fold. Even a systemic fever can be a problem. If your body temperature hits 40°C (104°F), the amount of fentanyl in your blood can jump by roughly 33%. While a fever alone might not always cause a full overdose, it significantly narrows your safety margin, especially if you're already close to your limit.
Dangerous Heat Sources You Might Overlook
Most people know to avoid a sauna, but there are several "hidden" heat sources that can cause an accidental overdose. It's not just about extreme heat; it's about any consistent increase in temperature at the site of the patch.
- Home Comforts: Electric blankets and heating pads are common culprits. Even a warm waterbed can increase the absorption rate over several hours.
- Beauty and Wellness: Tanning lamps, sunlamps, and long, steaming hot baths or showers are high-risk activities.
- Physical Exertion: Strenuous exercise raises your core temperature and increases blood flow to the skin, which can inadvertently accelerate drug delivery.
- Medical Settings: Warming blankets used during surgery can be dangerous if the medical team isn't aware the patient is wearing a patch.

Spotting the Signs of an Overdose
When fentanyl levels spike, the most immediate and dangerous effect is respiratory depression, where breathing becomes slow, shallow, or stops entirely. This is why heat exposure is considered potentially lethal.
You should watch for these red flags in yourself or a loved one:
- Extreme Sleepiness: Difficulty waking up or an inability to keep eyes open.
- Pinpoint Pupils: Pupils that remain very small even in dim light.
- Confusion: Mental cloudiness or disorientation.
- Physical Warning Signs: Clammy skin, slow heart rate, or a bluish tint to the lips and fingernails.
In some cases, patients might experience serotonin syndrome-marked by anxiety, muscle spasms, and sweating-especially if they are taking other medications that interact with the brain's chemistry.
Crucial Safety Rules for Patch Users
If you or a family member use these patches, following a strict set of rules is the only way to mitigate the risk. First, never use a heat source directly on or near the patch site. If you feel a fever coming on, call your doctor immediately to see if the patch needs to be removed or the dose adjusted.
Timing is also critical. Most patches must be removed exactly every 72 hours. It is a common misconception that the drug is "gone" once the patch is peeled off. In reality, a significant amount of fentanyl remains in the skin depot and continues to be absorbed for hours after removal. If you take a hot shower immediately after taking off a patch, you could still trigger a spike in drug levels.
Finally, be aware of medication interactions. Some drugs, such as certain antibiotics (erythromycin) or antifungals (ketoconazole), inhibit the enzymes in your liver that break down fentanyl. If you're on these medications, your body already struggles to clear the drug, making any heat-induced spike even more dangerous.
Can a hot shower cause a fentanyl overdose?
Yes, it can. Long baths or showers in hot water increase skin temperature and blood flow, which accelerates the absorption of fentanyl into the bloodstream. This can lead to dangerously high levels of the drug, increasing the risk of respiratory depression.
What happens if I have a fever while wearing a patch?
A fever increases your overall body temperature. Evidence suggests that a temperature of 40°C (104°F) can increase fentanyl serum concentrations by about 33%. You should contact your healthcare provider immediately if you develop a fever while using a transdermal patch.
Is it safe to use a heating pad on my back if the patch is on my shoulder?
While the heat is not directly on the patch, systemic warming can still affect absorption. However, the most acute risk is direct heat. The safest practice is to avoid all heating pads, electric blankets, and heat lamps while using these medications.
Why are fentanyl patches not used for acute pain?
Fentanyl patches are designed for patients who are already "opioid-tolerant." Because they deliver a high dose of a very potent drug, they could be lethal to someone who does not regularly take opioids (opioid-naïve patients), especially if absorption is accelerated by heat.
How long does the risk last after the patch is removed?
The risk does not end the moment the patch is removed. Fentanyl stays in the skin's upper layers as a depot and continues to be absorbed for several hours after the patch is gone. Avoid extreme heat immediately following removal.